Your skin has been quietly broadcasting distress signals long before your brain registers thirst. And if you know where to look, you can catch dehydration in its earliest, most correctable stage, no blood test, no doctor’s office visit required.
The spot in question is the back of your hand, or your forearm. And the test is so simple it almost seems too casual for a medical tool, which is exactly why most people never think to use it.
Key takeaways
- There’s a hidden dehydration alarm on your body that activates before you even feel thirsty
- A two-second pinch test on your skin can expose what your brain hasn’t noticed yet
- Even mild fluid loss shows up in your skin’s elasticity—but age changes the rules
The Pinch Test: A Clinical Classic You Can Do at Home Right Now
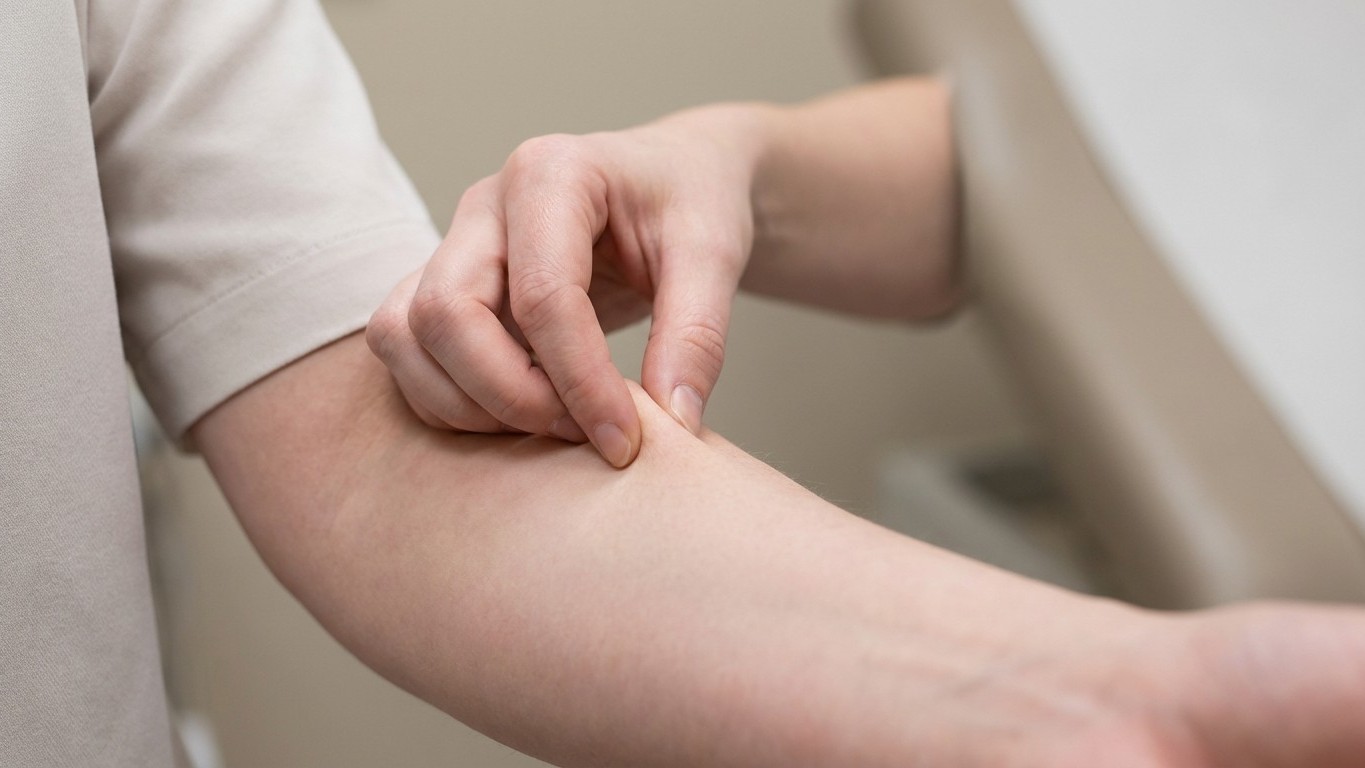
When you pinch your skin and it remains elevated instead of immediately bouncing back, you’re experiencing what medical professionals call “skin tenting” or poor skin turgor. This simple test, known as the skin turgor test or skin pinch test, has been used by healthcare providers for decades as a quick assessment of hydration status and skin elasticity.
Here’s how to do it properly. The healthcare provider grasps the skin between two fingers so that it is tented up. Commonly the lower arm or abdomen is checked. The skin is held for a few seconds and then released. Skin with normal turgor snaps rapidly back to its normal position. Skin with poor turgor takes time to return to its normal position. A crease that lingers for even a second or two is worth paying attention to.
The test works because healthy, well-hydrated skin contains adequate fluid in its cells and surrounding tissues, allowing it to quickly return to its normal position when released. Think of skin like a well-watered plant: the cells are plump, responsive, alive. Remove the water, and things start to droop, subtly at first, then unmistakably.
The counterintuitive part? If you feel thirsty, you’re already dehydrated. Thirst, that sensation we’ve been conditioned to treat as our hydration alarm system, is Actually a lagging indicator. The skin reveals the deficit first.
What’s Actually Happening Under the Surface
Your skin is 64% water. That number matters more than most people realize. The layers of your skin need moisture to work the way they’re supposed to. Without enough water, skin can’t Stretch or protect you as well as it should.
Dehydration is by far the most frequent cause of skin tenting. When your body lacks adequate fluids, it prioritizes vital organs over skin hydration, leading to decreased skin elasticity. Even mild dehydration of 2-3% body weight loss can cause noticeable skin tenting, along with other symptoms like dry mouth, decreased urination, and fatigue. That’s the part that should genuinely shift your perspective: a 2-3% fluid deficit is not a dramatic medical emergency, it’s an ordinary Tuesday afternoon when you’ve been in meetings and forgot to refill your water bottle.
This phenomenon is linked to tissue tension. Supple skin indicates good water distribution in the body. Conversely, sluggish or loose skin may suggest fluid loss.
And there are other signals your skin sends before the thirst alarm ever rings. One of the first signs of dehydrated skin is a lack of radiance. If your skin has lost its usual glow and appears lackluster, it may be lacking moisture. When the skin is dehydrated, it struggles to reflect light properly, leaving you looking tired even when you’re well-rested. This happens because dehydration affects the skin’s ability to renew itself, leading to a build-up of dead skin cells that dull your complexion. Dullness isn’t just an aesthetic complaint, it’s a physiological one.
The Age Factor (and Why the Back of Your Hand Can Mislead You)
Here is where the story gets more nuanced, and where the science pushes back a little on the “one-spot-solves-everything” simplicity.
As we age, our skin naturally loses elasticity due to decreased collagen and elastin production. This process, called elastosis, begins as early as our 20s but becomes more noticeable after age 40. The dermis layer of skin becomes thinner, and the connections between skin layers weaken, making skin tenting more common even with adequate hydration.
Aging skin also produces less hyaluronic acid, a molecule that can hold up to 1,000 times its weight in water. This reduction means that even well-hydrated older adults may experience some degree of skin tenting, making it important to consider age when interpreting skin turgor test results.
This is why location matters. The back of the hand is commonly used, but in elderly individuals, the forehead or sternum may provide more accurate results since these areas are less affected by age-related skin changes. For people in this age group, doctors recommend testing skin turgor over the sternum and on the forehead. These areas typically keep their natural skin turgor longer than others.
So the honest clinical picture: skin turgor measurement, whilst part of the initial assessment of children with suspected dehydration, is only moderately reliable and other clinical signs should be sought to confirm this diagnosis. Doctors use it as one piece of the puzzle, not the entire picture. That said, for otherwise healthy adults under 50 using it as a personal early-warning check, it remains genuinely useful, and accessible in a way that urine osmolality tests simply are not.
What To Do When Your Skin Signals the Alarm
The good news: mild dehydration is one of the most reversible conditions there is. You may see the signs of dehydration improve in as little as five to 10 minutes. The fix is rarely dramatic.
Drink small sips regularly throughout the day, even without waiting until you are thirsty; alternate between water, herbal teas, broths or semi-skimmed milk, which are sources of water and minerals; favor foods rich in water: salads, fresh fruits, compotes.
Eating water-rich vegetables and fruits can also help increase your intake, think celery, watermelon, and the like. Hydration, it turns out, is never just about what’s in your glass. You can also treat dehydrated skin with the following lifestyle changes: drink alcohol in moderation only (if at all); drink less coffee and other sources of caffeine.
One distinction worth keeping in mind: while dehydrated skin lacks water, dry skin lacks natural oils (also called sebum). Dry skin is a skin type, while dehydration is considered a condition. Reaching for a rich moisturizer when your body is actually craving water is a common and understandable mistake, but it won’t solve the underlying issue.
When should you stop trusting home tests and call a doctor? Severe dehydration, indicated by skin that remains tented for more than 2 seconds along with symptoms like confusion, rapid heartbeat, sunken eyes, or no urination for 8 hours, requires emergency care. That’s the threshold where self-monitoring ends and medical intervention begins.
For the rest of us, sitting at our desks, running errands, making it through a long flight on two sips of recycled air — the pinch test is a quiet, honest check-in. Your skin has always known things your brain hasn’t caught up to yet. The question is whether you’re paying attention.